Brain Imaging Techniques Provide Answers About Vegetative Patients
By Emma Yasinksi
BU News Service
In 2005, a serious car accident left a 23-year-old woman in a vegetative, unresponsive state.
For six months, she experienced sleep-wake cycles but was never able to communicate with her doctors and visitors. She couldn’t respond to simple commands such as “squeeze my hand,” or “look at this pen.”
Adrian Owen, Canada Excellence Research Chair in Cognitive Neuroscience at Western University, Canada wondered what was actually happening in her brain.
He slid her inside an fMRI, a machine that measures changes in the brain’s blood flow over time. Not knowing whether she could hear him, he told her to imagine she was playing tennis. He was excited to see that in response to his request, blood flow in her brain increased in the areas she would need to use to imagine herself playing the sport. While the blood flow in his patient’s brain was nowhere near that of a healthy individual, he felt that the increase was enough to indicate that she had heard him and was responding.
Over the past ten years, Owen’s “tennis test” has been replicated many times. Researchers have come to consider it a benchmark for studying vegetative patients, but it has never been applied as diagnostic tool. Now researchers are testing other imaging techniques that they hope will suggest which vegetative patients are most likely to awaken.
For now, clinicians are still using a scale developed in the 1970s to judge patients’ awareness based on their ability to respond to commands. The doctor will ask the patient to squeeze a hand, or look around the room. Then doctors use the responses to measure a patient’s diagnosis and likelihood of waking up on a scale which ranges from brain dead to conscious. Brain imaging studies using the tennis test have made it clear that doctors using behavioral methods are missing a group of patients who may be conscious but can’t respond to physical commands.
Up to 20% of patients who are diagnosed as vegetative using this scale actually pass the “tennis test,” according to Srivas Chennu, PhD, Senior Research Associate at Cambridge University, UK. This suggests that there is more going on in these patients’ brains than doctors might think.
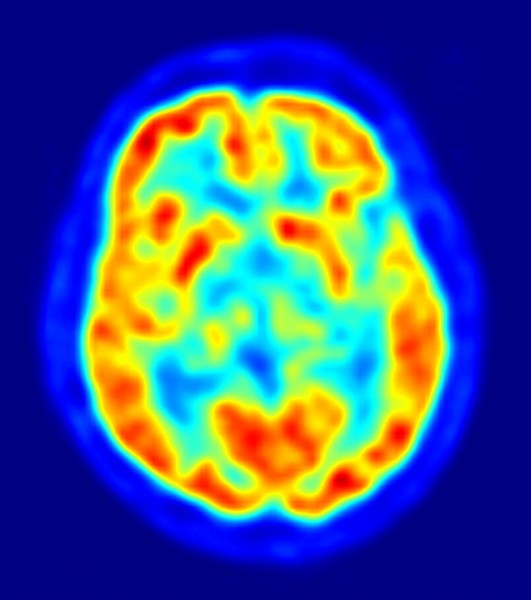
Researchers are exploring two main imaging techniques that measure brain activity in vegetative patients. The first is the PET scan, which measures glucose in the brain. Johan Stender, graduate student at the University of Copenhagen, and his team PET-scanned the brains of 126 patients who were vegetative or minimally conscious (inconsistently able to respond to commands,) without asking the patients to imagine anything. They followed the patients’ progress for a year, to see who regained consciousness. The team compared the results of the PET scans to the results of the fMRI tennis test on the same patients. Those patients who showed activity in the PET scan also passed the tennis test, and were the most likely to wake up within a year. According to the study, published in The Lancet in 2014, The PET scan correctly predicted who would wake up three out of four times. The authors recommended using the PET scans to complement behavioral tests when diagnosing vegetative patients.
Another group, led by Chennu, aimed to find the most convenient and cost-effective way to measure brain activity in vegetative patients. They used eletro encephylograms (EEG’s) – administered at the bedside with a cap and some electrodes – to measure the electrical activity in patients’ brains. The EEG showed that 4 of 13 vegetative patients showed much more electrical activity than the others. They found that these same four patients passed the fMRI tennis test, suggesting that the EEG could also distinguish this type of consciousness. They published the study in PLOS Computational Biology in October of 2014.
Although these results need to be confirmed in a larger study, it seems all three types of brain measurements may be able to help clarify diagnosis of vegetative patients and possibly predict who will wake up within the year.
In an effort to gain more information from the convenient EEG test, Chennu’s team used graph theory, a type of mathematics designed to measure systems and networks to measure the strength of the activity in the patients’ brains. With more research, these rankings may give even more detailed information about an individual patient’s diagnosis
“[Families] want to know what the diagnosis really is so that they can move on and deal with that. Doubt and uncertainty are always bad things.” Owen told Nature in 2012. As studies move forward and validate tools and help doctors understand their patients’ level of consciousness, the technology promises to help families cope with heart-wrenching diagnoses as well.
Leave a Reply